The American Cancer Society’s recently updated cervical cancer screening guidelines have drawn mixed opinions from doctors in the field.
On July 30, the society announced its updated recommendations to start screening at age 25, with primary human papillomavirus (HPV) testing as the preferred method of testing every five years through age 65. The previous guidelines, released in 2012, called for cervical cancer screening starting at age 21.
RELOCATING DURING THE PANDEMIC? BEWARE OF MOLD, EXPERTS WARN
These tests can help detect cervical cancer early.
During Pap tests, gynecologists swab cells near the patient’s cervix and send the sample to the lab to test for any abnormal or precancerous changes to the cells. For HPV tests, the doctor uses a small brush to collect cervical cells to test for HPV because certain high-risk HPV types can cause cervical cancer.
American Cancer Society officials said the update reflects a “rapidly changing landscape of cervical cancer prevention” in the U.S., and now calls for “less and more simplified” screening, according to a news release.
The change in the recommended age was also due to low cervical cancer incidence among those aged 20 to 24, and most HPV infections among these individuals become undetectable in one to two years.
Since not all labs have transitioned to primary HPV testing, the guidelines say acceptable options, for now, are HPV testing in addition to a Pap test (called co-testing) every five years, or Pap tests alone every three years.
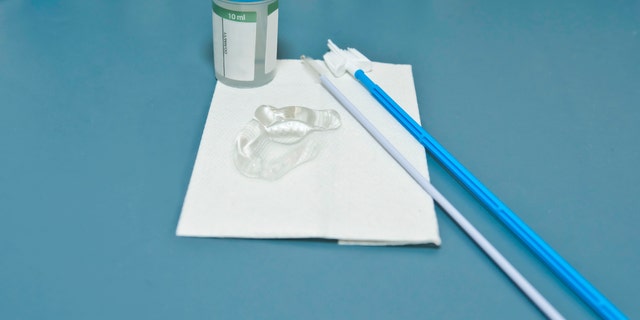
Since not all labs have transitioned to primary HPV testing, the updated guidelines say acceptable options are HPV testing in addition to a Pap test (called co-testing) every five years, or Pap tests alone every three years. Pictured is a pap smear medical test. (iStock)
However, some doctors say the changes are concerning and conflict with patients’ best interests.
Dr. Mark Spitzer, an OB/GYN specialist in New York and clinical professor of obstetrics and gynecology at Hofstra/Northwell Zucker School of Medicine, disagrees with the updated guidelines, arguing that co-testing earlier on is important for diagnosing cancer cases and saving more lives.
“Data clearly show that if you screen with two tests instead of one, screen more often and start at a younger age, you will discover and prevent a small, but a not insignificant number of additional cancer cases and save more lives,” Spitzer wrote in an email statement to Fox News. Spitzer is also a past president of the American Society for Colposcopy and Cervical Pathology (ASCCP).
However, Spitzer said co-testing at a younger age may detect some additional conditions that are not precancerous that, if treated with unnecessary colposcopies, may run the risk of preterm labor in a future pregnancy.
Dr. Jessica Shepherd, an OB-GYN gynecologic surgeon at Baylor University Medical Center, also spoke out against what she called “concerning changes” in the new guidelines.
“The guidelines recommend future removal of the Pap test, even though the Pap test remains a proven and effective part of the screening process. These guidelines are at odds with my belief that we should retain all screening options to best protect women’s health,” she added.
Before the society rolled out its new guidelines, the National Association of Nurse Practitioners in Women’s Health conducted a survey of 750 health care providers (HCPs) and 1,000 women on this topic and found that “the majority of HCP respondents continue to support the 2012 consensus screening guidelines that call for Pap testing for women ages 21-29 and co-testing for women ages 30-65.”
The survey results were published in June in Women’s Healthcare: A Clinical Journal for Nurse Practitioners.
Also, the survey said 61 percent of HCPs and 68 percent of women think that “eliminating the Pap test completely from frontline cervical cancer screening and only relying on HPV will have a negative impact on women’s health.”
The survey said 61percent of HCPs and 68 percent of women believe “that eliminating the Pap test completely from frontline cervical cancer screening and only relying on HPV will have a negative impact on women’s health.” (iStock)
After the American Cancer Society announced the updated guidelines on July 30, Dr. Christopher Zahn, vice president of practice activities at the American College of Obstetricians and Gynecologists (ACOG), issued a statement on the matter.
“ACOG looks forward to comprehensively reviewing the American Cancer Society recommendations and the supporting evidence in order to determine whether a similar update to our clinical guidance document on cervical cancer screening is needed,” he said.
“In the interim, ACOG affirms our current cervical cancer screening guidelines, which encompass all three cervical cancer screening strategies (high-risk human papillomavirus testing alone, cervical cytology alone, and co-testing),” he continued. “ACOG’s current screening guidelines reflect a balance of benefit and potential harms and support shared decision-making between patients and their clinicians.”
Asked for an update on ACOG’s stance on the issue, a spokesperson for the organization, Kate Connors, told Fox News that the ACOG does not have additional comments at this time.
However, “our clinical guidance is reviewed [every] 12-18 months, so our clinical review committees have not had [the] opportunity to evaluate the new information,” she noted.
Connors said the guidance remains in place.
MOTHER DIES AFTER HER CANCER IS PRESUMED TO BE CORONAVIRUS: REPORT
Dr. Michael Randell, an OB-GYN in Atlanta, Ga., echoed the sentiments of other doctors who disagree with the new guidelines.
“As a doctor, every decision I make is not only rooted in strong evidence but also in the patient’s best interest. This is how all patient care decisions should be approached,” Randell wrote in an email statement to Fox News. “The new American Cancer Society guidelines, however, do not support what data suggests is best for women and, therefore, do not put the patient’s interest at the forefront.”
Randell said the guidelines reduce choices for women and “reverse monumental advances” against cervical cancer — a preventable disease— ultimately putting more lives at risk.