The few hours it took to give the first coronavirus vaccine shots to 14 residents of the John XXIII nursing home — named after a pope and not far from the birthplace in eastern France of vaccine pioneer Louis Pasteur — took weeks of preparation.
The home’s director, Samuel Robbe, first had to chew his way through a dense 61-page vaccination protocol, one of several hefty guides from the French government that exhaustively detail how to proceed, down to the number of times (10) that each flask of vaccine should be turned upside down to mix its contents.
“Delicately,” the booklet stipulates. “Do not shake.”
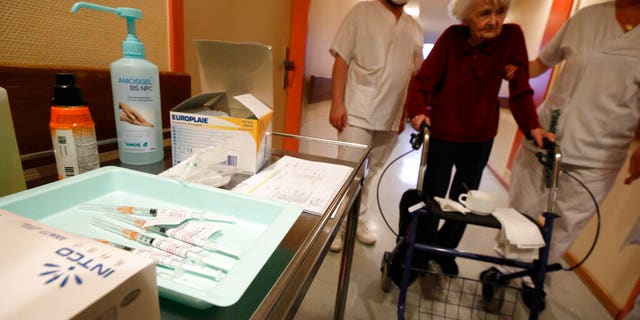
A resident is led to get the Pfizer-BioNTech COVID-19 vaccine at the Bois Fleuris nursing home in Strasbourg in eastern France, Jan. 6, 2021. (Associated Press)
As France tries to figure out why its vaccination campaign launched so slowly, the answer lies partly in forests of red tape and the decision to prioritize vulnerable older people in nursing homes. They are perhaps the toughest group to start with, because of the need for informed consent and difficulties explaining the complex science of fast-tracked vaccines.
Claude Fouet, still full of vim and good humor at age 89 but with memory problems, was among the first in his Paris care home to agree to a vaccination. But in conversation, it quickly becomes apparent that his understanding of the pandemic is spotty. Eve Guillaume, the home’s director, had to remind Fouet that in April he survived his own brush with the virus that has killed more than 66,000 people in France.
QUEEN ELIZABETH, HUSBAND PRINCE PHILIP RECEIVE COVID-19 VACCINATIONS
“I was in hospital,” Fouet slowly recalled, “with a dead person next to me.”
Guillaume says that getting consent from her 64 residents — or their guardians and families when they are not fit enough to agree themselves — is proving to be the most labor-intensive part of her preparations to start inoculations later this month. Some families have said no, and some want to wait a few months to see how vaccinations unfold before deciding.

<br>
Dr. Alain Guignon reads a prescription before getting the Pfizer-BioNTech COVID-19 vaccine in a clinic in Strasbourg, in eastern France, Jan. 5, 2021. (Associated Press)
“You can’t count on medicalized care homes to go quickly,” she says. “It means, each time, starting a conversation with families, talking with guardians, taking collegial steps to reach the right decision. And that takes time.”
At the John XXIII home, between the fortified town of Besancon and Pasteur’s birthplace in Dole, Robbe has had a similar experience.
MEMBER OF FAMED TUSKEGEE AIRMEN DIES FROM CORONAVIRUS
After the European Union green-lighted use of the BioNTech-Pfizer vaccine in December, Robbe says it took two weeks to put together all the pieces to this week vaccinate 14 residents, just a fraction of his total of more than 100.
Getting consent was the biggest hurdle for a doctor and a psychologist who went from room to room to discuss vaccinations, he says. The families of residents were given a week over the December holidays to approve or refuse, a decision that had to be unanimous from immediate family members.
<br>
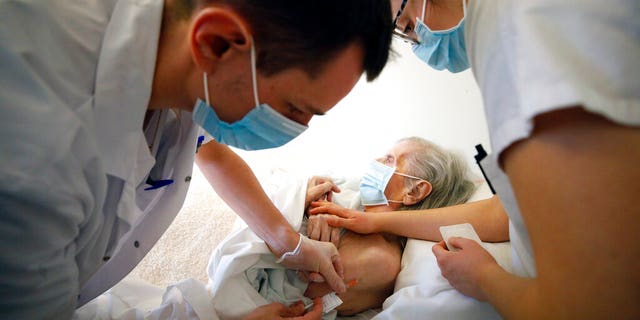
Dr. Cedric Waechter, left, administers the Pfizer-BioNTech COVID-19 vaccine to a resident of the Bois Fleuris nursing home in Strasbourg in eastern France, Jan. 6, 2021. (Associated Press)
When one woman’s daughter said yes but her son said no, a shot wasn’t given because “they can turn against us and say, ‘I never agreed to that,’” Robbe explained. “No consensus, we don’t vaccinate.”
Only by cutting corners and perfunctorily getting residents to agree could the process go quicker, he says.
NYC CLINIC FRUSTRATED BY CUOMO’S VACCINATION GUIDELINES GETS APPROVAL TO DISTRIBUTE UNUSED DOSES
“My friends are saying, ‘What is this circus? The Germans have already vaccinated 80,000 people and we’ve vaccinated no one,'” he says. “But we don’t share the same histories. When you propose a vaccine to Germans, they all want to get inoculated. In France, there is a lot of reticence about the history of vaccinations. People are more skeptical. They need to understand. They need explications and to be reassured.”
France prioritized nursing homes because they have seen nearly one-third of its deaths. But its first vaccination on Dec. 27, of a 78-year-old woman in a long-term care facility, quickly proved to have been only the symbolic launch of a rollout that the government never intended to get properly underway before this week.

A care home director, Eve Guillaume, gestures during an interview in Paris, Wednesday, Jan. 7, 2021. (Associated Press)
Only on Monday, as scheduled, did authorities launch an online platform where health workers must log all vaccinations and show that those inoculated got an obligatory consultation with a doctor, adding to the red tape.
In some countries that are moving faster than France, the bureaucracy is leaner. In Britain, where nearly 1.5 million have been inoculated and plans are to offer jabs to all nursing home residents by the end of January, those capable of consenting need only sign a one-page form that gives basic information about the benefits and possible side effects.
No doctor interviews are needed in Spain. It started vaccinating the same day as France but administered 82,000 doses in the first nine days, whereas France managed just a couple of thousand.
SERIOUSLY ILL CORONAVIRUS PATIENTS IN UK TO RECEIVE RHEUMATOID ARTHRITIS DRUGS
Germany, like France, also mandates a meeting with a doctor and is prioritizing shots for care home residents, but it is getting to them quicker, using mobile teams. At its current rate of nearly 30,000 vaccinations per day, Germany would need at least six years to inoculate its 69 million adults. But while the German government is facing criticism for the perceived slow rollout, France made an even more leisurely start, at least in numerical terms, but has pledged to reach 1 million people by the end of January.
Other countries have racked up bigger numbers by offering shots to broader cross-sections of people who are easier to reach and can get themselves to appointments. The large majority of the more than 400,000 doses administered in Italy have gone to health-care workers.
Lucile Grillon, who manages three nursing homes in eastern France, says the many hours invested to prepare vaccinations for 50 residents and staff who got jabs on Friday was time well spent. She worked through the holidays to get ready.
“We can’t wait until we have the doses in our fridge to realize that we’re not ready to vaccinate and then have to throw doses away and say, ‘Rats! I didn’t think of that,’” she adds. “The doses are too precious.”
CLICK HERE TO GET THE FOX NEWS APP
“It takes us two months to prepare for flu shots. Here, we have been asked to set records, to vaccinate against COVID in under 15 days,” she says. “I don’t see how we could have gone any quicker.”